It’s been a great 10 years
October 31, 2014
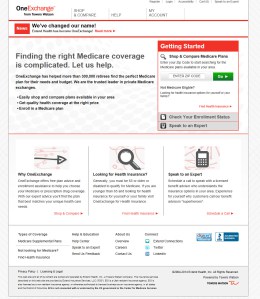
It’s hard to believe that it’s been nearly 10 years since my colleagues and I embarked on the journey of creating one of the nation’s first private exchanges. I’ve been privileged to be a part of the revolution as this important new industry has started to become a major force in how employers deliver health care benefits to all of their employee and retiree populations.
It’s been an amazing decade and the time is right for me to retire this blog as I move on to new ventures in health care and technology.
I look forward to continued conversations with many of you in my new venture at SeeChange, which will keep me closely tied to the world of health insurance.
I wish my colleagues and team members at Towers Watson all the best in these exciting times.
Companies Keep Coming Back
June 5, 2014
Very proud to have the confidence of these 50 employers and all our clients
OneExchange today marked an important milestone: 50 employer clients have used our private Medicare solution to transition multiple groups of customers.
Workforces can be complex, and changing benefits for multiple groups at once may not always be possible. Union contract negotiation timelines differ. Employers may want to test-drive a new approach like an exchange with a portion of their population first. And newly acquired companies may present an opportunity to streamline benefits administration after an initial group has already transitioned.
These are all reasons why employer clients have come back time and time again to OneExchange in addition to the reasons they chose Towers Watson’s Medicare solution in the first place.
71% of companies that offer retiree health care report that they already offer retirees access to a private…
View original post 54 more words
Pro Advice for CFOs: Exchanges as a Cost Management Tool
March 16, 2014
Skyrocketing health benefit costs have made cost management strategies a concern for every company officer. CFOs feel this acutely and are looking for solutions that transcend the traditional.
I spoke with three engineers of the next frontier of benefits delivery – chief actuary Dave Osterndorf, strategist Ben Pajak and active employee exchange expert Cathy Tripp – to get their best advice on how CFOs can leverage health insurance exchanges to tame health benefit costs now and down the road – when the stakes get even higher.
Here are their best thoughts on what’s driving the savings on exchanges, how much employers can expect to save and the impact on HR and benefits.
- What can exchanges really deliver?
- What about the Cadillac tax?
- What about so-called single-carrier exchanges?
- Is it realistic to expect the best health care price in every region?
- How can employers fund benefits on exchanges?
- What data and reporting can I expect to evaluate exchange effectiveness?
- What other issues do I need on my radar?
- Are there impacts to employee sentiment?
Question 1:
Cost management is the holy grail of health care right now. What can health insurance exchanges really deliver?
Osterndorf: There are significant opportunities for employers to save on health care coverage for active employees, which is why there’s a surge of interest in private health insurance exchanges. We’ve seen employers saving from 3% to 10% in their total spend, relative to their existing approach. Perhaps even more significant: Health care costs for employers using private exchanges are declining faster than costs for other organizations. Four factors are involved.
First, exchanges can offer multiple carriers in almost any geographic area, so employers can count on getting the best-negotiated deals in most locales. That’s quite different from working with one major insurance carrier to cover employees across the country. In that situation, companies could get the best deals in 70% or 80% of the geographies in which they operate, but could lag the market by as much as 5% to 10% elsewhere. In a private exchange, they get the best deals everywhere.
Second is the fact that exchanges have access to high-performance provider networks and can negotiate favorable prices in areas where those deals would be difficult for employers to do on their own.
Third, exchanges can structure plans progressively in the areas of plan design, and pharmacy and care management, and this can bring incremental savings every year.
And finally, joint purchasing efficiencies can help the employer, which benefits from the economies of scale associated with a large purchasing pool.
For example, it’s very challenging for an employer to build a best-in-class pharmacy program. An exchange can build a high-performance drug formulary that provides clinically appropriate drugs for all conditions, while using only the drugs that deliver the best outcomes for the money being spent. It takes market power and deep expertise to do that.
Question 2:
How does the so-called Cadillac or excise tax affect this picture?
Osterndorf: It will add to cost pressures. Starting in 2018, health benefit plans with premiums that exceed $10,200 for individuals or $27,500 for families will be taxed annually at 40% on each dollar above those figures. It’s a nondeductible tax, so even if an employer passes it through to employees, there will be negative tax consequences for the company’s financial reporting. At a minimum, an exchange for active employees must enable the employer to avoid having to pay that excise tax — which means keeping the cost of benefit offerings below the excise tax thresholds.
That won’t be easy. Come 2018, health plan cost trends will need to approximate the CPI, which has never before happened with health care costs. Employers need to feel confident that an exchange can achieve the required level of performance to reduce trend — not just for a single year, but over time. This is really a question of long-term sustainability.
There’s another important point about the excise tax that’s often misunderstood: It will be assessed on the total cost of the plan, including both employer payments and employee contributions. Employers can’t avoid paying the excise tax just by cutting back on their financial subsidy. An organization must be able to manage its plans exceedingly well to avoid the tax.
That’s really the issue finance executives need to quantify. Is their current path sustainable? If the answer is no, the employer must ask its potential exchange partners: How can you help us lower our cost trend for the foreseeable future? Where do the savings come from? And what data can you show us to help us understand the financials?
There is a sense of urgency in taking advantage of savings, since the sooner you can affect the slope of the trend line, the longer it may take to hit excise tax thresholds.
Question 3:
To achieve the cost savings we’ve discussed, employers will need to examine a number of important design elements. One is the carrier model: multiple versus single. Are there circumstances under which employers should consider a single-carrier model?
Pajak: It depends on where their employees are located and which plans are available in those locations. No single carrier offers the best discounts in every U.S. geographic area. But if your entire workforce is based in one location, a single carrier might deliver the best savings there. Even then, employees will appreciate having choice, which single-carrier models may not provide.
Another consideration is long-term cost mitigation. Carriers that cover multiple geographic areas tend to have sophisticated care management and wellness programs to help control costs over time.
Osterndorf: It’s tough to get added value with a single-carrier model, especially for active employees. Those models can provide a degree of additional choice, through networks or the underlying benefit structure, but most employers can provide those choices to employees without using an exchange. To ensure that moving to an exchange is worthwhile for the employer, the solution needs to bring significant incremental value.
Tripp: It’s useful to compare the two models from the employee’s perspective. With multiple carriers, employees choose a plan as well as the carrier with a network that includes the employees’ preferred physicians and services. With a single carrier, those decisions are forced upon them. If the employer switches from carrier A to carrier B, it can wreak havoc on employees who lose access to their physicians.
Question 4:
In a multiple-carrier situation, how can employers be sure they’re getting the best deal in every location where they have employees?
Tripp: As part of due diligence, employers should conduct a detailed cost analysis that shows the impact of the best-in-market pricing in the locations where they have employees. In a multicarrier exchange, this can bring significant savings for both the employer and the employee.
Question 5:
Let’s shift to another important plan element. What are the considerations in choosing a funding model, and what impact will that decision have on long-term health plan costs?
Tripp: Employers can self-fund or fully insure the arrangement. In deciding which approach to take, employers should consider their desired level of purchasing flexibility, their overall cost position and financial goals, and the importance of having predictable costs year after year. Today, the vast majority (94%) of large employers self-fund plans, and they want to maintain this funding model to preserve the purchasing efficiency their plan design affords. Others want the peace of mind that comes from knowing their total outstanding cost in any given scenario.
But shifting from a self-funded to an insured model brings a one-time double whammy. The employer must pay claims that were incurred under the self-funded plan but not paid yet. It also must prepay the fully insured equivalent rate, beginning in January. So in looking at the total cost, cash flow in that first year is a major consideration.
Osterndorf: When you move from a self-insured to a fully insured platform, you are accepting the additional costs of state premium taxes, the PPACA-mandated assessment and some additional administrative costs. The incremental cost of being fully insured, along with the risk-reduction premium that you pay to move from an unknown cost to a fully known cost, will total between 6% and 11% of your total health care spend. For some employers, that’s an acceptable premium. But for many that already have fairly predictable costs, it’s an added cost they don’t need.
One of the downsides of a fully insured approach is that it can be difficult to determine where the real savings are. You must understand how features like network configuration, pharmacy programs and care management work. Finance leaders looking at exchange offerings will want to understand exactly where those savings will come from. They should challenge the exchange operators to give them that information so they can do apples-to-apples comparisons.
But there are some scenarios where an employer may be willing to pay more to have the predictable costs that come with fully insured models. This can be true for small employers, those with business models that are less able to support the volatility of
self-funding and those for whom stop loss doesn’t offer enough certainty.
Question 6:
The ability to assess results is clearly crucial, in both selecting an exchange and monitoring its performance. What should employers expect in terms of data and metrics to ensure an exchange is delivering on its promises?
Tripp: Employers should expect standard financial reporting and reconciliation from a data warehouse containing information from all plans, at a minimum. However, a well-performing exchange should be able to show the choices employees are making in plans, how the health status of the overall workforce is changing and whether the promised savings are being realized.
The employer should ask the exchange: Are the plans delivering savings at the projected levels? Is Rx spending dropping as people make better choices? Is there less spending on people with chronic diseases because they’re getting better support?
Question 7:
When an employer considers moving to an exchange, what issues beyond cost come into play?
Osterndorf: Moving to an exchange is often both a health plan cost-control decision and a benefits administration outsourcing decision. For the CFO in particular, it comes down to the most effective deployment of resources: Can many things being done internally be done better externally? If they’re being done externally, can the employer redeploy internal resources for greater effectiveness? What do we give up, and what do we get?
CFOs commonly consider whether using external resources would improve quality and efficiency. Would that work for health care benefits? We think so.
An exchange provides many advantages, but employers do lose some control. Exchanges reduce the customization possibilities to the extent that they come with preset options. Some organizations are uncomfortable relinquishing control over health plan elements, and this can create tension between financial and administrative goals. This is where close collaboration between the organization’s finance and HR executives will make a difference in both making the right decision and facilitating an effective transition to an exchange.
Tripp: There’s a trust issue involved as well. Moving from an employer’s self-managed plan to an exchange-managed solution typically means shifting from a one-to-one relationship with a carrier you’ve come to trust to a one-to-many relationship with the exchange and its array of carriers. That array is part of why the exchange can leverage its purchasing power across multiple clients. But it also means the exchange makes most of the design and carrier decisions to benefit all of its members, not just one employer.
Pajak: Exchanges allow the employer to rethink its use of resources and reconfigure plan administration. This could include anything from technology to who takes on day-to-day plan management. Employers need to examine the promised value and opportunities associated with each exchange operator. And then explore combining those elements with their management approach to improve the value proposition for the organization and its constituents, and to reduce the hard- and soft-dollar costs of delivery.
Question 8:
Some employers are concerned about possible employee reactions. What are the issues and risks in this regard?
Pajak: The most important thing is to ensure that employees have access to appropriate levels of care, as well as financial protection in the case of an unfortunate personal event. With those elements in place, there’s typically minimal negative impact on workforce morale and productivity. The experience for employees will be similar to what it is today, but with added choice. And if the exchange’s efficiencies reduce costs for all parties, the message is even more positive.
Osterndorf: Another consideration is how the employer will interact with its workforce. For example, when you transition Medicare-eligible retirees to private exchanges, you move them from the world of group health insurance to the individual marketplace. You discontinue many ongoing conversations you’ve been having with that workforce segment. For many employers, that’s good because they aren’t (and don’t want to be) Medicare experts. And devoting time and focus to the retiree population doesn’t help leaders manage the business.
It’s different when you move active, full-time employees to an exchange. While you no longer manage the program’s daily operations, you still play a significant role in various other aspects of employee health and health care benefits, including communication and providing supportive programs.
A crucial goal for any health care program is to effectively address the health needs of the active population. An exchange must help you minimize the business risks of an unhealthy workforce and maximize employee health and productivity. If it can’t do those things, that exchange probably won’t help you run your business more effectively.
Here’s what CFOs need to remember:
This reinforces the importance of considering exchanges in the context of your organization’s business strategy. Judging an exchange’s value comes down to three questions:
- Can the exchange help you achieve the desired financial outcomes in the short and long terms?
- Where will the savings come from?
- Does the exchange promise enough value to justify making the change?
OneExchange Headlines Towers Watson’s Exchange Offerings
February 24, 2014
Check out our new look as Towers Watson’s OneExchange.
 Find out more about OneExchange
Find out more about OneExchange
Welcome to our new look! The OneExchange blog.
The blog’s new name and face reflect changes that began over a year ago when Towers Watson launched OneExchange.
Building on our private Medicare exchange roots, this blog has expanded to include news, research, trends and insights for all workforce populations – from full-time and part-time employees to pre-65 retirees in addition to our original Medicare perspective.
See OneExchange everywhere
You can see the new OneExchange look at all our sites, including:
- On Twitter:
- @OneExchange– Check out the new face of our tweet stream.
- @brycewatch –
 Follow us on Twitter at @OneExchange & @BryceWatch
Follow us on Twitter at @OneExchange & @BryceWatch Check out the latest from our managing director, Bryce Williams, at his tweet stream.
- Online:
- medicare.oneexchange.com – Check out the new face of our private Medicare exchange
Towers Watson Announces Expansion of Exchange Solutions Segment
January 25, 2014
Jim Foreman to lead Exchange Solutions, Carl Hess to succeed Foreman as managing director of Americas Region
In a move designed to help employers better navigate the dynamic health care environment, global professional services company Towers Watson announced plans to unite the company-wide expertise and resources dedicated to health care exchanges and administration within its Exchange Solutions segment.
My thoughts: “Health insurance exchanges will play a significant role in how employers deliver health care benefits to their employees and families in the future. And as the marketplace evolves, I look forward to continuing to work with the Exchange Solutions team to deliver the best possible solutions to our clients.”
Listen in: My comments to NPR on the first days of the ACA plans
January 25, 2014
I joined a panel of experts on exchanges, health care reform and insurance to give insights on ACA plans going into effect. To The Point tweeted key comments from each of us, including:
- Bryce Williams, Towers Watson, @brycewatch:
The ACA could be major boost to entrepreneurship - Sarah Kliff, Washington Post, @sarahkliff:
36 hrs into Obamacare, vast majority can signon & signup w/in an hr - Susan Shargel, Shargel and Company
- David Nather. Politico, @DavidNather
- Gerald Kominski: UCLA Center for Health Policy Research, @UCLAFSPH
In the full podcast, you’ll hear comments on these points and more:
The New Year brought with it medical coverage for millions of Americans under the Affordable Care Act. On Jan 1, about two million people began to receive private health coverage through the state health exchanges or the federal website.
With one of the nation’s most sweeping changes to social policy in decades, no longer can insurers deny coverage to people with pre-existing conditions, or charge them more for their coverage than other customers. It’s also the first time they can’t legally charge women higher premiums for the same coverage as men, and the first time they can’t set a specific limit on the amount they spend on “essential health benefits” for individual policyholders.
But there are a lot of “if’s” in the implementation of Obamacare:
- Will people be able to find a doctor who accepts their new plan?
- Are the nation’s healthcare providers ready for the change in policy?
- How will Obamacare shape the political climate this election year?
Sharing Team Pride: Healthcare’s Hottest & Industry Innovator
November 30, 2013
I’m proud to share some recognition in the fields of health care business and consumerism.
 Modern Healthcare: 2013 Healthcare’s Hottest Companies
Modern Healthcare: 2013 Healthcare’s Hottest Companies
The Exchange Solutions segment of Towers Watson, launched with the acquisition of Extend Health, was recognized by Modern Healthcare for being one of the fastest growing health care companies in the U.S. – named 4th among a great group of companies.
Institute for HealthCare Consumerism: 2013 Innovator > See pg 63
 I’m honored to be named among some very esteemed industry figures by the Institute for HealthCare Consumerism. See page 63 to learn a little about the early days of Extend Health and what’s it’s meant to my team at work and at home to be in the leading wave of health insurance exchanges in our nation.
I’m honored to be named among some very esteemed industry figures by the Institute for HealthCare Consumerism. See page 63 to learn a little about the early days of Extend Health and what’s it’s meant to my team at work and at home to be in the leading wave of health insurance exchanges in our nation.
Get a Closer Look at Towers Watson’s Liazon Acquisition
November 23, 2013
I spoke with several journals about what the Liazon acquisition means for Towers Watson and the exchange space. This coverage pulls in opinions from across the industry as well as my highlights.
![]() Private Health-Exchange Market Consolidates, David McCann
Private Health-Exchange Market Consolidates, David McCann
My highlight: “Towers Watson has plenty of good reasons for buying Liazon….The market is moving so rapidly, and there’s a sense that a tipping point is being achieved…It’s as if the music just stopped and we grabbed the last chair.”
![]() Towers Watson expands private exchanges with $215M Liazon purchase, Jerry Geisel
Towers Watson expands private exchanges with $215M Liazon purchase, Jerry Geisel
My highlight: “Liazon has “the most sophisticated insurance platform by a mile in this market.”
![]() Towers Watson’s private exchange division leader details advantages of Liazon purchase, Kathleen Koster
Towers Watson’s private exchange division leader details advantages of Liazon purchase, Kathleen Koster
My highlight: “We want to be the leading player in private exchanges….A year and a half ago, they [Towers Watson] bought the leading retiree exchange in Extend Health. Today, they’re buying the leading active exchange technology company, Liazon….The acquisition gives Towers Watson the ability to hit the market very quickly with all the most sophisticated exchange technology out there.”
More on the acquisition
- Towers Watson’s announcement
- Reuters
- Wall Street Journal
- Huffington Post Business
- Bloomberg BusinessWeek
- Daily Finance, Motley Fool
- Insurance Networking News
- Employee Benefit Advisor
- LifeHealthPro
- Plan Sponsor
A closer look at Liazon
- New York Times, The Landscape of Small-Business Health Insurance
- FastCompany, This Buffalo Startup Built the Amazon of Health Care Buying
Towers Watson Acquires Liazon to Expand Private Benefit Exchange Offerings Through Multiple Channels
November 22, 2013
Transaction complements Towers Watson’s OneExchange with scalable, flexible solution
NEW YORK, November 22, 2013 — Towers Watson (NYSE, NASDAQ: TW), a global professional services company, announced today that it has acquired Liazon Corporation, a leader in developing and delivering private benefit exchanges for active employees. The acquisition, which follows the purchase of Extend Health in June 2012, solidifies Towers Watson’s strength in the private exchange market through its OneExchange solution. Going forward, Towers Watson will continue to enhance Liazon’s award-winning private exchange solution and serve the needs of Liazon’s leading broker, consultant and carrier partners, some of which offer the Liazon product under their own brands.

Warren Olney hosts me among a panel of exchange and health care reform experts to give insight on week 1 of the ACA exchange roll-out
This morning I had the chance to speak with Warren Olney and a group of other exchange and health reform experts on the first days of the ACA exchange roll-out.
I joined a panel of experts on when the ACA will be ready for prime time. To The Point tweeted key comments from each of us, including:
- Bryce Williams, Towers Watson: Hard to penalize Americans for not buying what they can’t easily buy online says @brycewatch
- Juliet Eilperin, Washington Post White House correspondent: WH has stopped giving reporters like @eilperin hard #s about Obamacare web hits
- Jyoti Bansal, AppDynamics: Healthcare.gov glitches partly due to “old legacy systems” from state websites says @appdynamics
- Peter Suderman, Reason magazine: Whopping 7% polled say Obamacare roll-out has gone “quite well” says @petersuderman
- Tayse Haynes, Cabinet for Health and Family Services of Kentucky: One surprising state where Obamacare’s been less rocky: Kentucky. We hear from the health czar.
In the full podcast, you’ll hear comments on these points and more:
- What factors states had to consider in setting up their exchanges
- What could happen with those who get their coverage later due to state exchange glitches
- How options for young people’s coverage could impact state exchanges
- How this launch compares to the roll-out of Medicare Advantage and Part D nearly a decade ago